I’ve been thinking for a while that I’d like to write my birth story, as it’s one of those things you don’t want to bore people with in real life too often but it percolates around your own head for a long, long time after the event. There have been two shoulder dystocia births on One Born Every Minute recently and it’s been quite upsetting to watch them as it’s been a reminder of just how lucky we were. This story might be a bit gory but it has a happy ending, promise.
Just over a week before my due date on a Saturday evening I was sitting on the loo at home, trying to wee quickly so I wouldn’t miss the start of X Factor, when there was a very audible popping sound, quickly followed by a gush of water. I called out to DH that my waters had broken and his response, ‘Are you sure?’ made me laugh-there was definitely no mistaking it. Contrary to popular belief fuelled by Hollywood, labour doesn’t often start with your waters breaking but there was no way this could be anything else. I put on one of those giant maternity pads that only add to your inability to walk properly at that stage in a pregnancy, realised it was full within seconds of standing up, sat back down, tried again and repeated the process a few more times. (Yep, still gushing. I thank God I was on the loo when this happened. I’d been having nightmares over the previous few weeks that it would happen in the middle of Waitrose.) Eventually I managed to get up to call Triage. They like you to go in to be checked out as lots of people think their waters have gone when they’ve actually just had an accident, though I was pretty confident I was right about this one! We went in, giant maternity pads strewn all over the car, and a midwife had a look at a pad. (Given the rest of their job I’m sure they don’t mind doing this but the idea of examining someone else’s maternity pad is pretty gross to me. She didn’t seem to mind though.) She confirmed it was my waters and sent us home to wait for the contractions to start. She warned us that if nothing had happened by Monday morning I’d have to go in to be induced, as once the waters have gone the risk of infection for the baby goes up significantly.
We got home, settled back in front of X Factor (that’s a looooong show) and wondered excitedly whether we’d have a baby by morning. At about 11pm I started to get a few contractions. They weren’t bad and felt just like strong period pains that came and went every 20 minutes or so. We went to bed and I managed to sleep a bit but not much, as every time I started to drift off I’d have another contraction and wake up. At some point in the small hours I fell asleep properly and when I woke up in the morning I realised it was because the contractions had stopped.
By about 11am they’d started up again and this time they didn’t stop. They built up over the course of the day but never got past a rate of about 2 every 15 minutes which, I can tell you, is the precise rate of contractions that will annoy the hell out of you as you’re unable to do or think about anything else, but not a rate that a midwife will care about as you need 3 every 10 minutes to be deemed interesting. We spent about 2 hours walking round and round the block to try and encourage them along but it didn’t do much. FINALLY by bedtime they started heating up and I spent another night awake, but this time pacing around the sitting room timing contractions and willing them to speed up. My Hypnobirthing classes were pretty useful by this point and I was breathing and walking, breathing and walking. DH went to bed (I sent him to be honest-one of us needed some sleep!) and I woke him up at about 4am as the contractions were upping in intensity and were finally coming 3 in 10. The breathing was still working and I was feeling pretty good, if knackered.
We grabbed our bags (which had been packed for a fortnight!) and drove to the hospital. They put us in a room with an ensuite bath and gave me a birthing ball to bounce on too, and after a little bit came to examine me. By this point we’d reached the point where if I wasn’t in full blown labour they’d want to induce me as it had been 36 hours since my waters had broken. I’d been contracting for most of the weekend so I was fairly confident I’d be quite dilated…erm, WRONG. I had dilated by a measly 2cm. IN 36 HOURS.
Midwife no 1 told us I couldn’t have a water birth (which I was really upset by) as it had been too long since my waters had gone and that I needed to be induced by a drip. We said we’d rather wait. She got annoyed. We got annoyed. For the record, we didn’t want to be induced for a couple of reasons:
1) if you’re induced you’re statistically likely to have more interventions such as forceps/c section etc, which didn’t fit with our idea of a hypno/waterbirth.
2) I had heard that because induction ramps up your contractions so swiftly the pain increases exponentially and I wanted to avoid an epidural as I wanted an active birth and didn’t want to be on my back.
She agreed to give us another few hours to see if my body could get going on its own (and probably went to warn the other midwives that I was a grumpy cow!). By about 4pm I was still only 2cm dilated and had started to go into shock, I think due to the length of time I’d been awake and the worry that my body wasn’t playing ball. At one point I was in the bath and my whole body was shaking uncontrollably which was quite scary. When the midwife said I needed to be induced now, we agreed. We were taken into a labour room, handed over to midwife no 2 and I was given the dreaded epidural.
Unfortunately the person trying to do my epidural (who must have been a student, looking back) hit bone the first couple of times she tried and eventually had to call a consultant to come and guide her through the process. The whole thing was terrifying and very stressful as all I could think about was the fact that an incorrectly administered epidural can paralyse you! In the end it was in and they started up the drip in my hand. (Same lady-and she messed that one up too so the bruising was pretty bad and I couldn’t move my fingers properly for a couple of days. Lovely.)
The epidural was an interesting experience. Midwife no 2 asked whether I could feel anything and kept topping it up because I could still feel pain in various parts of my stomach. The contractions weren’t painful for a couple of hours and then it wore off and they were really fucking painful. The midwife kept telling me it was normal to feel pressure but not pain and I don’t think quite believed me when I said it was real pain I could feel. I was using my breathing again and also gas and air to get through them. (Awesome stuff. Makes you feel like you’re floating.)
I’d always thought that pushing was something you had to actively do, and that with an epidural you’d have to be told when to do it as you wouldn’t feel your contractions. This wasn’t the case at all for me-for a start I could feel everything and, in addition, I couldn’t have stopped the pushing if I’d tried. My body just did it. It was bloody painful but the breathing and gas helped, and it didn’t take long before the midwife (no 3 by now) said she could see the baby’s head. Within a couple of pushes the head was out and she was telling me that just one more push and we’d meet our baby. It took a few minutes, however, of big pushes and nothing changing before she went a bit pale and asked DH to press a button on the wall. Another midwife quickly came in, had a quick look and pressed the button again. Within seconds there were about 15 people in the room, plus a tiny baby crash cart. DH was pushed into the corner of the room (and left there, not knowing what was going on-something he said was the most terrifying thing that’s ever happened to him as he was convinced DD was dying or dead) and two midwives grabbed my knees and held them down by my ears while someone else made a fist and punched hard on my lower stomach several times. At this point I’d been awake and contracting for about 50 hours so I was pretty out of it and didn’t really register what was going on. With one final punch DD was yanked out and whisked onto the cart where she spent a hideous minute not breathing. Once she’d been resuscitated and checked for broken bones and paralysis (both common injuries due to the pressure put on the shoulder by the punches) she was finally given to me to hold and everyone left us alone. The midwife was very shaken and said to us that we’d been very lucky as if the McRoberts manoeuvre and suprapubic pressure hadn’t worked I’d have needed an emergency c-section, which there probably wouldn’t have been time for. (Given that DD’s head was out it would have been bloody difficult too! Given also that I could feel everything due to the epidural having worn off I try not to think about the possibility of a c-section. I’m sure they’d have topped it up, but it generally didn’t seem to work well on my body.)
Shoulder dystocia, where the baby’s shoulder is stuck behind the mother’s pelvis, is pretty rare and can be deadly. Babies don’t start to breathe until their lungs have been squeezed out and as the baby’s head is out but the lungs aren’t that can’t happen in these instances-combine that with a squashed placenta and you quickly have a baby with no oxygen supply. However, although it’s an emergency, and a pretty terrifying one at that, midwives in this country are very well trained and we were so grateful to have the wonderful, speedy, efficient, calm and careful care that we had. Midwife Pam, you are our hero.
It’s more likely to happen if a) the baby is very large (she wasn’t), b) it’s happened to you before (nope-first baby) or c) you have a very long labour and are induced.
This website, American Family Physician, has some good info:
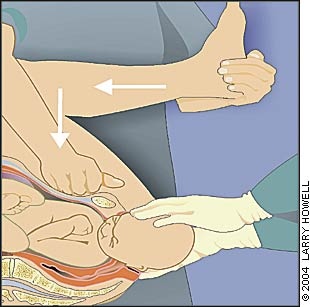
Shoulder dystocia can be one of the most frightening emergencies in the delivery room. Although many factors have been associated with shoulder dystocia, most cases occur with no warning. Calm and effective management of this emergency is possible with recognition of the impaction and institution of specified maneuvers, such as the McRoberts maneuver, suprapubic pressure, internal rotation, or removal of the posterior arm, to relieve the impacted shoulder and allow for spontaneous delivery of the infant. The “HELPERR” mnemonic from the Advanced Life Support in Obstetrics course can be a useful tool for addressing this emergency. Although no ideal manipulation or treatment exists, all maneuvers in the HELPERR mnemonic aid physicians in completing one of three actions: enlarging the maternal pelvis through cephalad rotation of the symphysis and flattening of the sacrum; collapsing the fetal shoulder width; or altering the orientation of the longitudinal axis of the fetus to the plane of the obstruction. In rare cases in which these interventions are unsuccessful, additional management options, such as intentional clavicle fracture, symphysiotomy, and the Zavanelli maneuver, are described.
Shoulder dystocia is one of the most anxiety-provoking emergencies encountered by physicians practicing maternity care. Typically defined as a delivery in which additional maneuvers are required to deliver the fetus after normal gentle downward traction has failed, shoulder dystocia occurs when the fetal anterior shoulder impacts against the maternal symphysis following delivery of the vertex. Less commonly, shoulder dystocia results from impaction of the posterior shoulder on the sacral promontory.1
The overall incidence of shoulder dystocia varies based on fetal weight, occurring in 0.6 to 1.4 percent of all infants with a birth weight of 2,500 g (5 lb, 8 oz) to 4,000 g (8 lb, 13 oz), increasing to a rate of 5 to 9 percent among fetuses weighing 4,000 to 4,500 g (9 lb, 14 oz) born to mothers without diabetes.2–4 Shoulder dystocia occurs with equal frequency in primigravid and multigravid women, although it is more common in infants born to women with diabetes.2,5 Several additional prenatal and intrapartum factors have been associated with an increased incidence of shoulder dystocia (Table 1). The single most common risk factor for shoulder dystocia is the use of a vacuum extractor or forceps during delivery.2 However, most cases occur in fetuses of normal birth weight and are unanticipated, limiting the clinical usefulness of risk-factor identification.6
We were so lucky to have a healthy baby at the end of it all, and I was also very lucky to only have a 2nd degree tear (3rd or 4th degree can happen with shoulder dystocia) which was easily stitched. I’m fairly sure that the reason DD refused point blank to breast feed (for 10 heart wrenching and exhausting days before we cut our losses and switched to formula) was because of the trauma of the birth, though I’ll never know for sure. I’m very nervous that if we have a second baby it’ll be more likely to happen again, and one of the suggestions is to have an elected c-section, but I’m pretty much petrified of those too (it makes me think of medieval torture, which I’m aware is ridiculous) so there’s a lot of thinking to be done! Ultimately though, we’re so privileged to have one happy, healthy child, and we’re so grateful for that.
Read Full Post »







